A cephalohaematoma is an accumulation of blood under the scalp that results from minor trauma during the birth process. They are common, occurring in 1-2% of all deliveries.
The blood collects between the periosteum and the skull and is hence, defined by the boundaries of these structures- it does not cross the midline or suture lines, as demonstrated in Image 1.
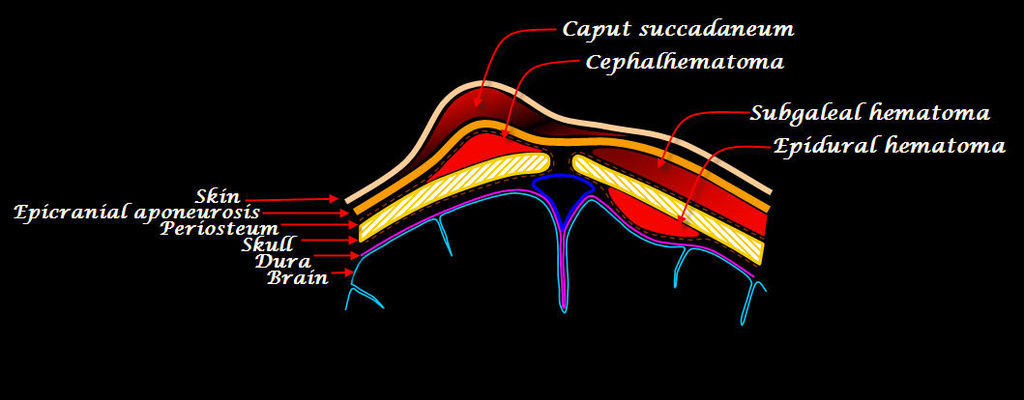
Image 1. Anatomical basis for appearance of scalp haematomas
During the birth process there is rupture of the blood vessels crossing the periosteum due to the pressure on the fetal head when passing through the birth canal or from the use of forceps or vacuum deliveries.
Cephalohaematomas are generally not present at birth and develop in the hours to days after the birth. Scalp haematomas presenting outside of this timeline need to be carefully evaluated for other causes e.g. NAI, vascular or lymphatic abnormalities.
Cephalohaematomas generally don’t require any treatment. Reassurance and parental education are the cornerstones of management. The natural history of cephalohaematomas should be explained to the parents. They can take weeks to resolve as the clotted blood slowly gets absorbed. The blood may calcify and the area may become firmer but they will eventually resolve.
Infants with a cephalohaematoma are at increased risk of jaundice due to increased haemolysis and should be monitored for this.
Rarely, cephalohaematomas may become infected. The most common organism is E.coli. (2) Infections due to S.aureus, Group B streptococcus, Proteus and other organisms may also be seen. Risk factors for infection include bacteraemia with secondary seeding and overlying cellulitis.
References
Cephalohematoma – StatPearls – NCBI Bookshelf [Internet]. [cited 2020 Aug 20]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470192/
Wang JF, Lederhandler MH, Oza VS. Escherichia coli-infected cephalohematoma in an infant [Internet]. Vol. 24, Dermatology Online Journal. Dermatology Online Journal; 2018 [cited 2020 Aug 20]. Available from: https://pubmed.ncbi.nlm.nih.gov/30695981/
